-
SCOTT MINIEA's advice for those who haven't yet taken advantage of the Affordable Care Act's current open enrollment period: "things change, so...it's…
-
The Missouri Senate is considering a bill that would extend Medicaid for new mothers struggling with addiction, a notable expansion for a state that did…
-
Today Paul Pepper visits with Welcome Home's TIM RICH about the many services available to homeless veterans in our community, because they need more than…
-
More than 200 people gathered to voice their concerns about health care at a town hall on Tuesday night hosted by CoMo for Progress.The town hall was held…
-
Health care policy has come back into public discussion in a big way, and we want to add your voice to the conversation. Over the coming months, we’ll be…
-
A lunchtime rally brought about 50 people to U.S. Senator Roy Blunt’s Columbia, Missouri office Friday, voicing their support for the Affordable Care Act…
-
When Joe Morris had a heart attack last Easter and had to be rushed to the ER, it was the first time he’d been to the doctor in more than 40 years —...
-
Prosecutors are moving forward with a case against 23 clergy members involved in a 2014 protest of the Missouri Senate.Authorities charged the clergy with…
-
Jeremy Milarksy sits behind his office computer and opens up the calendar of appointments for the week. There’s hardly any white space. Appointments are…
-
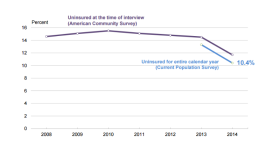
The number of uninsured residents in Missouri and throughout the U.S. is down, according to the 2014 American Community Survey. The United States Census…
Play Live Radio
Next Up:
0:00
0:00
Available On Air Stations